
Introduction
Insurers today face a stark challenge: customers demand instant, 24/7 service for complex, high-stakes interactions like claims submissions and policy renewals, yet traditional call center models can't keep pace. The median cost per contact for assisted channels reaches $13.50, while self-service options cost just $1.84—a 7.5x gap that makes legacy models unsustainable as query volumes grow.
AI agents represent a purpose-built solution to this pressure. Unlike older rule-based chatbots that follow rigid scripts, modern AI agents use large language models and agentic reasoning to understand policyholder intent, access backend insurance systems, and complete multi-step service tasks autonomously. That includes filing a First Notice of Loss, processing policy changes, and delivering real-time claim status updates without human handoff.
This guide covers:
- Core use cases driving AI agent adoption in insurance
- Measurable business benefits backed by industry data
- A phased deployment roadmap for insurers
- Criteria for selecting the right platform for your organization
TL;DR
- AI agents handle end-to-end insurance queries by accessing policy data, initiating actions, and completing workflows—not just answering FAQs
- Top use cases: claims intake and tracking, policy information queries, renewal reminders, new customer onboarding, and fraud flagging
- Insurers see measurable gains: faster claim resolution, lower cost-per-contact, and higher satisfaction scores
- Successful deployment depends on core system integration (CRM, CMS, claims platforms) and a phased rollout with defined KPIs
- Key selection criteria: NLP accuracy for insurance terms, omnichannel reach, compliance guardrails, and system integration depth
What Are AI Agents for Insurance Customer Service?
AI agents in the insurance context are software systems that use large language models (LLMs) and agentic reasoning to understand customer intent, access backend insurance systems, and complete multi-step service tasks autonomously. Unlike basic chatbots that answer FAQs from a script, AI agents can verify a policyholder's identity, retrieve their policy details, file a claim, collect required documentation, and send confirmation—all without human intervention.
Traditional chatbots follow fixed decision trees: "Press 1 for claims, press 2 for billing." If a customer's query falls outside the script, the bot fails. AI agents reason through problems dynamically—handling policy lookups, claim status updates, document collection, and coverage explanations by pulling live data from policy management systems and adapting responses based on context.
For insurers processing thousands of daily interactions, this means handling more volume with the same team, while maintaining consistent, accurate responses across every channel.
Agentic AI vs. Basic Chatbots: What's Different?
The core architectural difference lies in planning and action. Gartner defines agentic AI by its capacity for autonomous action—the ability to act autonomously to complete tasks and proactively resolve service requests on behalf of customers—with the firm projecting 80% autonomous resolution of common service issues by 2029.
Basic chatbots respond to inputs but don't plan sequences of steps. An AI agent, by contrast, executes a full workflow:
- Verify the customer's identity using their policy number and date of birth
- Retrieve active policy details and check relevant coverage
- Initiate a claim by collecting incident information
- Send a confirmation email with the claim reference number
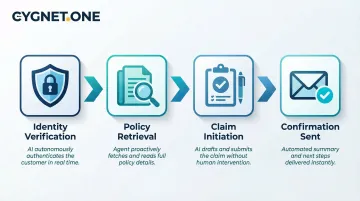
This planning capability is what makes AI agents effective for complex insurance workflows. They don't just provide information—they complete transactions, update records, and move processes forward across claims, renewals, and policy servicing.
Key Use Cases: How AI Agents Are Transforming Insurance Customer Service
Claims Intake and Status Tracking
AI agents accelerate the most resource-intensive part of claims operations: First Notice of Loss (FNOL) intake. They handle the full intake sequence:
- Guide policyholders through initial claim submission
- Collect required documentation (photos, police reports, medical records)
- Validate submissions against policy terms
- Provide real-time status updates throughout the claims lifecycle
UK insurer Aviva reduced liability assessment time by 23 days and cut customer complaints by 65% by deploying over 80 AI models in its claims domain. Allianz's 'Project Nemo' reduced processing and settlement time for eligible small claims by 80%, shrinking the timeline from days to hours.
The business impact is clear: faster claims resolution improves customer satisfaction while reducing the volume of "where's my claim?" calls that consume adjuster time. An estimated 40% of inbound call volume in claims departments consists of basic claims status checks—queries AI agents can handle instantly.
Policy Information and Coverage Queries
High-volume, repetitive policyholder questions—deductibles, exclusions, renewal dates, premium breakdowns—are ideal for AI automation. AI agents pull live data from policy management systems to answer these queries accurately, freeing human agents to focus on complex cases requiring judgment or empathy.
Traditional call centers route all inquiries to human agents regardless of complexity. AI agents triage automatically: simple queries get instant resolution, while nuanced questions—disputes, coverage interpretations—escalate to licensed agents. Routine requests close faster; high-stakes interactions get the human attention they need.
Renewal Reminders and Cross-Sell/Upsell
AI agents proactively contact customers before policy expiry via SMS, email, or chat, reducing lapse rates and creating revenue opportunities. They surface relevant upgrade options based on coverage history. A customer who recently purchased a new vehicle might see a prompt for higher liability limits; a policyholder in a flood-prone area gets a targeted add-on recommendation.
Beyond retention, AI agents generate revenue by identifying cross-sell opportunities that human agents often miss under time pressure. By analyzing policy history and customer behavior, they surface personalized recommendations across thousands of policies simultaneously.
New Customer Onboarding
AI agents reduce friction during onboarding by walking new policyholders through document submission, KYC verification, coverage explanation, and first-payment setup. This reduces drop-off rates—a critical metric for insurers competing in digital channels.
AI-native insurers like Lemonade demonstrate the potential: customers can purchase a policy in under 90 seconds. While traditional insurers face legacy system constraints, AI agents still deliver measurable improvements by automating manual steps, validating documents in real-time, and providing instant responses to onboarding questions.
Fraud Detection Support
Insurance fraud costs businesses and consumers at least $308.6 billion annually. AI agents act as a first-line filter by flagging inconsistencies in claim submissions—unusual patterns, duplicate filings, mismatched information—and escalating suspicious cases to Special Investigations Units (SIU) for human review.
Catching fraud at intake—before investigative resources are committed—reduces both financial exposure and case backlogs. AI agents don't replace fraud investigators; they focus investigator attention on the highest-risk claims, improving both speed and precision of fraud response.
Business Benefits of AI Agents in Insurance Customer Service
24/7 Availability and Faster Resolution
AI agents eliminate hold times and after-hours service gaps by resolving common queries instantly, at any time. Allstate's conversational AI achieves a 38-40% containment rate, fully resolving nearly four out of ten digital conversations without human intervention.
For claims processing specifically, the speed gains are dramatic. Aviva's AI deployment reduced complex case assessment time by 23 days, while Allianz's Project Nemo cut small claim settlement time by 80%. Customers get answers when they need them, not when an agent becomes available.
Significant Cost Reduction Per Interaction
AI agents handle high-volume, low-complexity interactions at a fraction of the cost of human agents. Assisted channels cost $13.50 per contact, compared to $1.84 for self-service—a 7.5x difference that compounds quickly at scale.
For insurers processing thousands of daily interactions, this translates to millions in annual savings. AI agents allow customer service organizations to scale without proportional headcount growth, redirecting budget toward complex case resolution and customer experience improvements.

Improved Customer Satisfaction and Retention
Faster resolution, proactive communication, and personalized responses directly improve customer satisfaction scores. An insurer using intelligent automation for sales saw customer satisfaction scores (likelihood to refer) rise by 36 percentage points.
The satisfaction gain comes from meeting what customers actually expect: fast answers and proactive updates without requiring them to call in.
When policyholders receive claim status notifications automatically, or when renewal reminders arrive with tailored coverage recommendations, they experience the insurer as attentive rather than reactive.
Empowering Human Agents to Focus on Complex Cases
AI agents work alongside human agents, not in place of them. By absorbing tier-1 and tier-2 queries, they free human staff to concentrate on the interactions that actually require their expertise.
The downstream effects are measurable:
- Human agents spend less time on repetitive queries and more time resolving complex issues
- Customers with straightforward questions get instant answers without waiting in a queue
- Policyholders facing disputes or coverage gaps receive focused, undivided attention
- Agent morale improves when work shifts from script-reading to genuine problem-solving
How to Deploy AI Agents for Insurance Customer Service
Step 1 — Identify and Prioritize Automation Opportunities
Start by auditing current customer service interactions by volume and complexity. Create a deployment priority matrix:
High Volume + Low Complexity = Strong AI Candidate
- Claims status checks
- Policy information queries
- Payment confirmations
- Renewal reminders
High Complexity + High Empathy = Human-Led
- Coverage disputes
- Claim denials requiring explanation
- Policy cancellation requests
- Complaints escalation
Focus initial deployment on high-volume, low-complexity interactions where AI agents can deliver immediate ROI while building organizational confidence in the technology.
Step 2 — Integrate with Core Insurance Systems
AI agents must connect to policy management systems, claims platforms, CRM, and document management tools to deliver real value. Without system integration, AI agents are limited to generic Q&A: they cannot access customer-specific data or complete transactions.
Successful integration typically spans four areas:
- Policy administration systems for coverage details and renewal dates
- Claims management platforms for FNOL intake and status updates
- CRM systems for customer history and interaction logging
- Document management systems for collecting and validating claim documentation
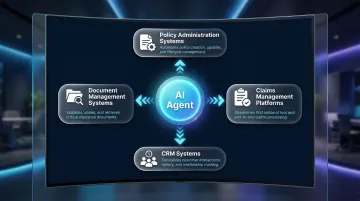
Pre-built API connectors and established integration frameworks significantly reduce implementation time at this stage — particularly for insurers running legacy policy administration systems.
Step 3 — Configure for Compliance and Escalation
Insurance is a regulated industry. AI agents must operate within clear boundaries:
Regulatory Compliance:
- Train AI on what it cannot advise on without a licensed agent (policy recommendations, coverage interpretations)
- Maintain audit trails for all customer interactions
- Ensure data handling complies with applicable privacy regulations
Escalation Triggers:
- Define scenarios requiring immediate human handoff (complaints, claim disputes, high-value policies)
- Build escalation workflows that route complex cases to appropriate specialists
- Test escalation paths to ensure seamless transitions without customer frustration
Step 4 — Test, Measure, and Iterate
Deploy in phases: pilot on one channel first (web chat), measure performance, refine, then expand to additional channels (phone, mobile app, email, WhatsApp).
Measuring success at each phase requires clear metrics from the start. Track the following KPIs:
- Containment rate (percentage of queries resolved without human handoff)
- Customer satisfaction (CSAT) scores
- Average handle time
- Cost per resolution
- First-contact resolution rate
Establish a feedback loop to continuously retrain the AI agent on real insurance queries. Monitor edge cases where the AI struggles and use those examples to sharpen its insurance-specific responses.
How to Choose the Right AI Agent for Insurance Customer Service
Evaluate NLP Accuracy and Insurance Domain Knowledge
General-purpose AI agents often lack insurance-specific vocabulary and scenario coverage. Look for platforms trained on—or adaptable to insurance data: policies, claims language, and regulatory terminology.
That domain coverage needs proof, not just a sales pitch. Ask vendors for task-specific accuracy benchmarks on insurance queries, then request pilot testing on your actual customer service data before committing to full deployment.
Check Omnichannel Support and System Integration Depth
Insurers serve customers across phone, web chat, mobile apps, email, and WhatsApp. The right AI agent must work across all channels and integrate natively with core insurance tech—policy admin systems, claims management platforms, CRM—or gaps in data will surface the moment a customer switches channels.
When evaluating vendors, check for:
- Pre-built connectors for common insurance and BFSI systems
- API-first architecture that supports custom integrations
- Documented implementation timelines from comparable insurance deployments
Assess Compliance Safeguards and Escalation Design
In a regulated industry, the AI agent must have built-in guardrails:
- Cannot provide unlicensed financial advice
- Clear human handoff flows for complaints and claims disputes
- Full conversation logging for audit purposes
- Role-based access controls for sensitive customer data
Test escalation workflows during the pilot phase. The AI should recognize when it has reached the limits of its authority and route the customer to a human agent—without the customer having to repeat themselves or restart the conversation.

Frequently Asked Questions
What is the best AI for insurance agents?
The "best" AI depends on your specific needs: claim volume, channels used, and integration requirements. Strong solutions combine NLP accuracy for insurance terminology, direct integrations with policy and claims systems, omnichannel support, and compliance controls for regulated interactions.
Are insurance companies using AI customer service?
Yes. 76% of U.S. insurance executives have already implemented Generative AI in one or more business functions, with claims handling and customer service as common deployment areas. Major insurers use AI agents for claims intake, policy queries, renewal management, and fraud flagging.
How to choose the right AI agent?
Prioritize domain-specific NLP for insurance language, core insurance system integrations (policy admin, claims, CRM), omnichannel reach (web, mobile, phone, email), compliance features (audit trails, escalation triggers), and the vendor's proven BFSI track record.
What tasks can AI agents automate in insurance customer service?
The highest-impact automatable tasks include claims status updates, policy FAQs, FNOL intake, renewal reminders, document collection and validation, basic premium calculations, and coverage eligibility checks—any high-volume, low-complexity interaction.
How do AI agents handle complex insurance claims?
AI agents manage initial intake, documentation collection, and status updates, but complex or disputed claims escalate to licensed human agents. This keeps routine claims moving quickly while ensuring disputed or large-payout cases get the human judgment and licensed expertise they require.
Will AI agents replace human insurance agents?
No. AI agents augment rather than replace human agents. They handle high-volume routine interactions—freeing human agents to focus on complex, empathy-intensive, and high-value policyholder relationships that require judgment, negotiation, or licensed expertise.


